Acting swiftly to save sight
Macular degeneration (MD) no longer sentences patients to functional blindness, but early diagnosis and referral is crucial, as are optometrists as the front-line eye health care providers who can educate, refer and support.
Company director Ross Legh was at a “boring” board meeting in Australia when he decided to test his sight using a makeshift Amsler grid – it was a move that saved his sight.
“I’d been diagnosed with drusen about 12 years before and told they were an indicator for macular degeneration,” he explains. “I was given an Amsler grid by ophthalmologist Dr Dianne Sharp who explained how to use it and told me to check my sight regularly.”
At home, Legh put the grid up on his bathroom mirror and used it to check for signs of MD every four to six weeks. “My wife even used it, although she’s not at risk. It just became routine, a part of our life. Although I didn’t let it worry me.”
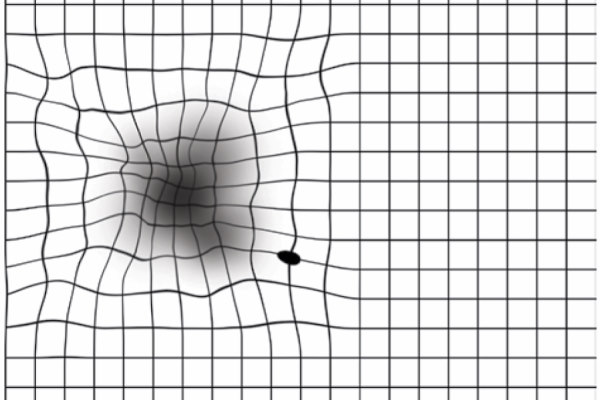
On that fateful day four years ago in Sydney, Legh didn’t have his Amsler grid but he noticed the pattern of the window mullions on the building opposite was like an Amsler grid. Carefully, he covered his left eye. “My right eye was fine, so I switched to my left.” Distressingly, Legh noticed that the grid-style lines on the building were distorted.
“I flew home that night and went straight to my optometrist the next day,” recalls Legh. “Tests were inconclusive, and he said, ‘there might be something going on’, but he was happy to monitor it for now. He suggested I come back in a few months.”
Legh, however, was not happy and requested a referral to Dr Sharp.
“It was a Thursday and I made an appointment for the following week. But (Dr Sharp’s office) phoned back a little while later to make it earlier as Dr Sharp had seen the report from my optometrist and was concerned.”
Legh had several tests and was advised he had wet macular degeneration in his left eye.
“Of course, I was worried, I knew it was serious and I was concerned how vision loss might affect me. Could I still run my business, take part in my hobbies? Dr Sharp advised me that left unchecked I could lose my sight in that eye within two years. That was terrifying.”
Legh began monthly treatment with the newer-generation anti-vascular endothelial growth factor (anti-VEGF) drug aflibercept (Eylea) almost immediately in the hope of preserving his sight. Incredibly, not only has he kept his vision, it has actually improved, and he now needs just four maintenance injections a year.
Now a trustee for MD New Zealand (MDNZ), Legh says he believes the role of an optometrist is to give every single patient over 55 an Amsler grid and show them how to use it. If a patient comes back worried about their Amsler grid results, refer them to an ophthalmologist straight away, he says.
But an optometrist’s role doesn’t stop at diagnosis, notes Legh, as patients require their ongoing support with compliance and understanding. “Remind them to go for their treatment. Help them understand the lifestyle changes that can improve or maintain vision. Tell them about MDNZ so they can get the emotional and practical support they need.
“Unfortunately, if I had taken my optometrist’s advice and waited a few months, I probably would have lost the sight in my left eye. MD is the leading cause of blindness in New Zealand, but It shouldn’t be. It’s important everyone knows as the treatments are so good now and there is so much support for those who have already lost vision. There is no reason to hold back at all. If you suspect wet MD, refer a patient on immediately.”
Time lost means vision lost
“The key factor in Ross’ outcome is that he knew what to look for,” says Dr Dianne Sharp from Retina Specialists. “About a decade before, I had diagnosed him with soft drusen. We talked about the risks and over the next 10 years he monitored himself regularly and sought help quickly when he noticed a change.”
Dr Sharp says all patients with soft drusen should be educated on how to monitor their own vision for change and that’s something optometrists can do. Soft drusen, termed intermediate age-related MD, have a 50% risk of progressing to late MD (wet AMD or atrophic AMD) over five years.
“Now we have good treatment options we must act rapidly,” she says. “We know the treatment works best if vision is not too severely affected at presentation. Time lost means vision lost.”
It’s also important for optometrists to note that although there is no treatment for dry or atrophic MD, patients can be helped by low vision specialists, says Dr Sharp. “Magnification, contrast and lighting advice is essential, as well as making sure they have a good support system in place. Whether a patient has wet or dry MD there is always something we can do to help and the Blind Foundation are a great support system if they are eligible for registration”
Five steps to help your MD patients
- Give every patient over 55 an Amsler grid and show them how to use it, especially if they have risk factors. Encourage regular self-monitoring.
- If a patient has recent onset of distortion or inconclusive symptoms, refer them immediately. Waiting a couple of months to see how things progress could negatively affect their outcome.
- Educate patients about lifestyle changes that could improve their prognosis. MDNZ has information about exercise, diet and supplements that could be helpful.
- If a patient has been diagnosed with wet AMD, check to make sure they are attending their ophthalmology appointments and adhering to treatment plans.
- Advise patients with MD to contact their local macular degeneration support organisation for further help for them and their families.