Indentation, OCT and more gonioscopy
The 2019 Eye Institute conference workshops day once again proved popular with most of the limited places snapped up well before the day and the rest exceeded by those who turned up unexpectedly.
Many attendees had travelled from across the country to Auckland to attend the workshops, saying they were a highlight of their conference calendar due to their small size and hands-on nature.
OCT 101
The first workshop was given by one of Eye Institute’s retina specialists, Dr Narme Deva who provided a practical take on the ups and downs of optical coherence tomography (OCT). The workshop was supplemented by a handy OCT Cheat Sheet, penned by her colleague Dr Shanu Subbiah who was busy helping with the gonioscopy workshops.
With more than 70% of attendees acknowledging they now had an OCT in their practices and the others saying they were soon to get one, the OCT 101 workshop provoked a lot of practical questions. A key thing to remember when you look at an OCT scan is that you’re seeing virtual anatomy, “how it reflects back at you, not actual anatomy,” said Dr Deva, adding dilation is important as “you’re only as good as the quality of the scan you do.”
Dr Deva’s other tips included always using the same machine and scanning the same area to monitor progression, the need to look for outer retinal pathology, practice makes perfect and questioning whether the scan fits what you know about a patient. “Correlate what the patient is complaining about with what you scan for on an OCT.”
Indentation
Dr Peter Hadden, aided by Dr Nick Mantell, then donned his indirect ophthalmoscope and put dilation drops in everyone’s eyes to tackle the practicalities of scleral indentation. The procedure can cause corneal abrasions and lacerations, so he didn’t recommend it unless absolutely necessary, he said. In his experience, it’s also not really required for seeing retinal tears, which then led to a discussion about which holes lead to retinal detachments and when to refer.
If checking for holes, get everything in your favour, said Dr Mantell. “Ideally use a darkened room, dilate the pupil and lie the patient flat so you can see their periphery better… and, if you’re worried about the signs and symptoms, ask someone.”
Gonioscopy
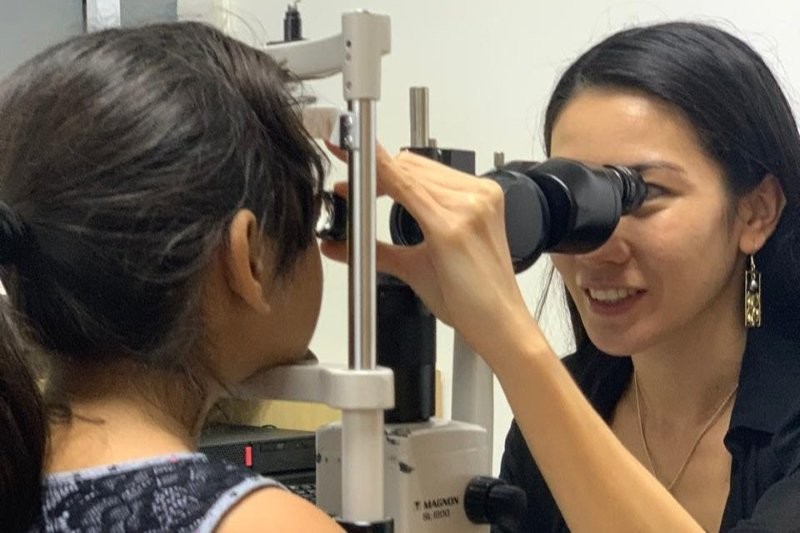
Back by popular demand, the third 2019 Eye Institute workshop once again tackled gonioscopy, essential for diagnosing and monitoring the glaucoma forms and progression.
Most New Zealand ophthalmologists and hospitals use the Shaffer grading system, which describes the degree to which the angle is open rather than the degree to which it is closed, said Dr Jay Meyer before providing a very practical, hands-on gonioscopy workshop to the delight of attendees.