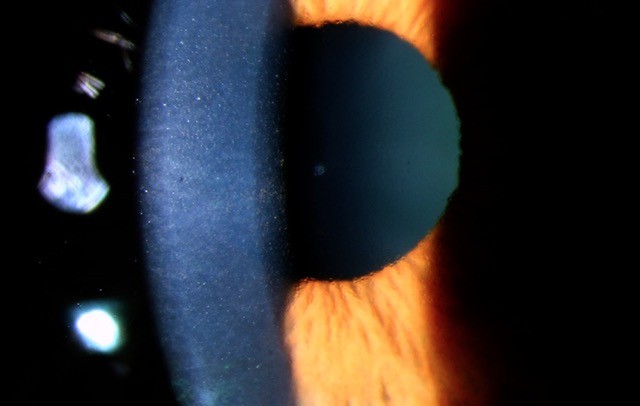
Optic disc, drusen OCTs and idiopathic intracranial hypertension
The role of OCT in differentiating optic disc drusen from oedema
Costello F, Malmqvist L, Hamann S
Asia Pacific Journal of Neuro-Ophthalmology 2018; 7: 271-279
Review:
This article describes in detail the role of optical coherence tomography (OCT) in diagnosis and monitoring of papilloedema and optic disc drusen. Different parameters of OCT scans in patients with papilloedema and disc drusen are discussed, including retinal nerve fibre layer thickness (RNFL), ganglion cell layer and inner plexiform layer (GCIP) thickness, Bruch membrane morphology, size of scleral canal, retinal and choroidal folds/wrinkles, enhanced depth imaging OCT scan (EDI-OCT) and peripapillary hyperreflective ovoid mass-like structures (PHOMS).
The main message of the article is that none of the above parameters are diagnostic on their own of either optic disc drusen or papilloedema and should be used as ancillary tests in combination with history and clinical examination to help physicians differentiate between the two.
Of special interest is a section describing PHOMS relation to papilloedema and disc drusen and the fact they have been erroneously diagnosed as disc drusen in several recent publications, creating confusion as to what exactly they represent. The authors assert them to be herniating, distended axons that could be seen in a variety of acquired and dysplastic optic discs as well as in papilloedema and disc drusen.
Comment:
This is a good summary on the utility of OCT for diagnosis and monitoring of patients with papilloedema and disc drusen and in particular the difficulties encountered in attempting to differentiate between mild cases of papilloedema and disc elevation due to buried drusen. The issue of PHOMS, what they represent and their relation to disc drusen, is actively being debated in the current literature.
Multimodal imaging of buried optic nerve head drusen
Wang DD, Leong JCY, Gale J, Wells AP
Eye 2018; 32: 1145-1156
Review:
This is a concise article attempting to clarify OCT findings in cases of buried disc drusen. Authors describe observational findings in five patients with buried disc drusen that were diagnosed clinically and confirmed by ultrasonography.
Both hyperreflective and hyporeflective structures were found in peripapillary regions of the same optic nerves. Hyperreflective structures (termed peripapillary hyperreflective ovoid mass-like structures or PHOMS in other studies) did not show autofluorescence, whereas smaller hyporeflective ones did demonstrate localised autofluorescence.
The authors hypothesise that larger hyperrflective structures (PHOMS) represented obstructed axoplasmic material and smaller hyporeflective structures represented calcified disc drusen composed of degenerated extracellular mitochondria.
Comment:
This paper, among others, shows the co-existence of hyperreflective (what is now termed PHOMS) and hyporeflective (buried disc drusen) structures within the peripapillary area as seen on an OCT scan of the optic nerve head. An issue of definition of what buried optic disc drusen represent is raised and will no doubt be debated in the literature over the next several years.
A population-based evaluation of the association between hormonal contraceptives and idiopathic intracranial hypertension
Kilgore KP et al.
AJO 2019;197:74-79
Review:
This article is a retrospective, case control study which examined a multicentre medical records’ database on all patient-physician encounters in Olmsted County, Minnesota, USA and reviewed medical records of all female patients with a diagnosis of idiopathic intracranial hypertension (IIH) from 1990 to 2016. IIH’s main symptoms are headaches and visual factors, including blind spots, poor peripheral and double vision and temporary and permanent vision loss.
In the study, 53 females aged from 15 to 45 were diagnosed with IIH. The use of the oral contraceptive pill (OCP) and other hormonal contraceptives in patients with IIH was compared to age, sex and body mass index (BMI) to matched controls. The study found 20.8% of patients with IIH used hormonal contraceptive at the time of diagnosis compared to 31.3% of controls. The odds ratio for hormonal contraceptive use and IIH was 0.55 (p=0.174).
The authors concluded there was no significant association between OCP or other hormonal contraceptive use and a higher incidence of IIH. They recommended not to discontinue hormonal contraceptives in women with IIH.
Comment:
The relationship between hormonal contraception and IIH has been controversial for several decades due to conflicting results from a number of studies over the years, most of which suffered from some form of methodological flaw. This current study provides further support to the notion that hormonal contraceptives do not result in increased risk of IIH.
Dr Taras Papchenko is a consultant ophthalmologist at Auckland Eye and Greenlane Clinical Centre. He graduated from Auckland Medical School in 2002 and received his PhD in ophthalmology in 2013 after which he spent two and a half years in the UK sub-specialising in oculoplastic surgery and neuro-ophthalmology.