TFOS survey of DED diagnosis patterns
Diagnostic and subclassification testing of dry eye disease (DED) is particularly important for informing tailored and optimised management plans for patients in clinical practice, as well as for guiding participant recruitment and the evaluation of outcome measures in population-based epidemiology studies and clinical trials1,2. Nevertheless, the 2017 Tear Film & Ocular Surface Society (TFOS) DEWS II workshop reports identified considerable variation and heterogeneity in dry eye diagnostic and subclassification methodology in existing literature1.Therefore TFOS conducted an international online survey to assess clinical practice patterns in DED diagnostic and subclassification testing.
The survey questions were devised by a panel of three internationally recognised DED specialists and TFOS members: Professor James Wolffsohn from Aston University, UK; Professor Jennifer Craig from Auckland University, New Zealand; and Professor Lyndon Jones from the University of Waterloo, Canada. The survey was distributed to eyecare practitioners in 51 countries, with responses collected between 2018 and 2019.
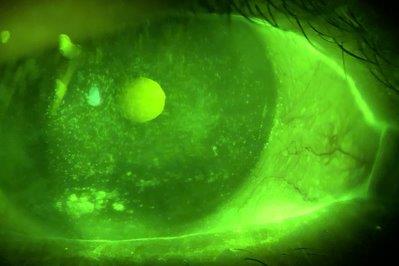
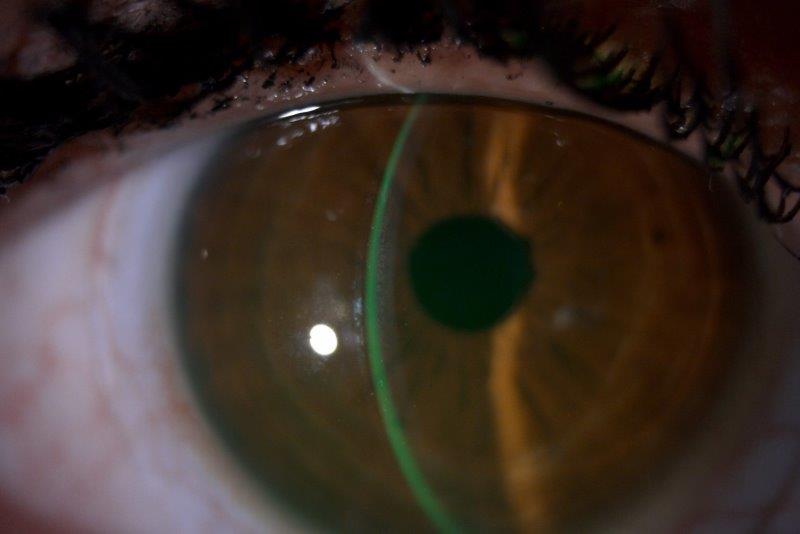
Overall, responses were obtained from a total of 1,139 eyecare practitioners. Of the respondents, 36% were ophthalmologists and 56% were optometrists. The results showed that a median of seven clinical tests were applied in the diagnostic workup of patients suspected of DED. The most common diagnostic tests included non-questionnaire-based symptom assessment, fluorescein breakup time and corneal staining, which were all used by more than 60% of respondents. The most popular subclassification tests included meibum expressibility and meibomian gland orifice examination for evaporative DED and Schirmer’s or phenol red thread test for aqueous deficiency, with these tests used by just over 30% of respondents.
Interestingly, a number of diagnostic and subclassification instruments recommended as part of the global consensus TFOS DEWS II criteria were less commonly used, including validated symptomology questionnaires, non-invasive tear film breakup time, tear osmolarity, lipid layer interferometry, infrared meibography and tear meniscus height1. However, it was acknowledged that the survey was conducted within two years of the release of the TFOS DEWS II reports, so it is hoped that increased adoption of the global consensus recommendations will be reflected in future surveys.
References
- Wolffsohn JS, Arita R, Chalmers R et al. TFOS DEWS II Diagnostic Methodology report. Ocul Surf. 2017;15(3):539-574.
- Jones L, Downie LE, Korb D et al. TFOS DEWS II Management and Therapy Report. Ocul Surf. 2017;15(3):575-628.
Dr Michael Wang, a neuro-ophthalmology clinical research fellow based at the University of Auckland and Sonia Trave Huarte, a doctoral student from Aston University, Birmingham, England, were both involved in this study, together with Professors James Wolffsohn, Jennifer Craig and Lyndon Jones.