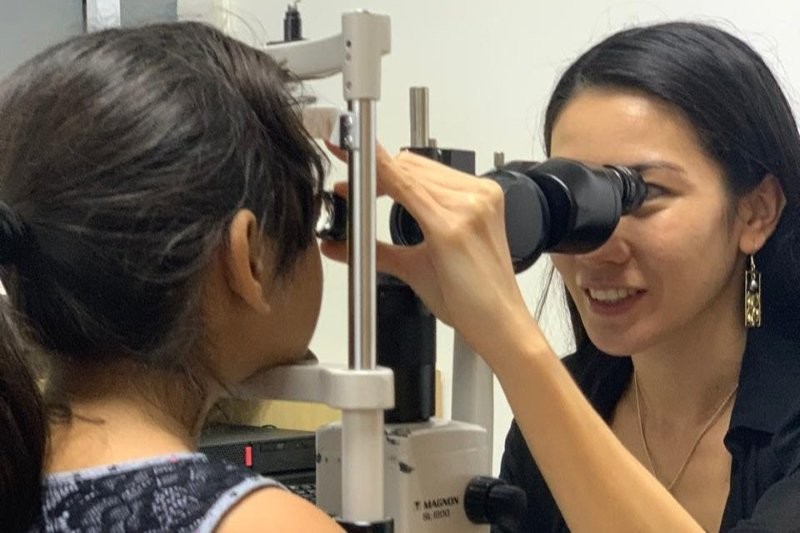
The aging nurse, apps and more at AONAVIC
We may mock our Australian neighbours, especially when it comes to cricket and sandpaper, but their ophthalmic nurses sure know how to put on a conference. Saturday 14 September in Melbourne was the 2019 Australian Ophthalmic Nurses Association Victoria Inc (AONAVIC) state conference, which includes South Australia and Tasmania.
For us out-of-towners it all started on Friday evening with an informal session at the public Royal Victorian Eye and Ear Hospital, co-hosted by the Centre for Eye Research Australia. After a warm welcome from President Heather Machin, we had a tour around the Lions Eye Donation Service / Eye Bank. Over 40,000 patients were seen in 2017-2018, including otorhinolaryngology patients. Yes, there are more to the ears and the nose than holding up glasses! It was also eye opening to see how their emergency department is still in action amid building and renovation.
The conference was like a smorgasbord (one of those healthy Swedish ones that my dad would tell me about) of mostly 15-minute presentations - nice bite sized talks. The overall themes were improving patient outcomes and meeting patient needs with different models of care, and education and future planning for ophthalmic nurses. Speakers came from all over the world, including UK-based ophthalmic nurse Lynne Hadley, president of the International Ophthalmic Nurses Association. A mix of ophthalmic and non-ophthalmic nurses and other staff from Australia. the Pacific and Titch Chan, Sue Raynel and myself from New Zealand made up the conference contingent.
Lynne’s presentations on the nurse-led botox and dystopia management clinic that she runs and The aging nurse, linked clinic management and education themes. Nurse-led clinics have been proven to be an effective way of meeting patients’ needs in a timely manner, along with other advantages, but how do we upskill nurses to do this? Lynne said there had been a skill service change in the UK (and in New Zealand too) and although the UK has developed future apprenticeship programmes for nurses, ophthalmology is a tiny section under physiological science. So, training ophthalmic nurses is tricky when we cannot even get nurses into ophthalmology!
Billy Ngai’s presentation on his ophthalmic nurse education in The Graduate Nurse Program: The QEH Example was most positive. Billy went straight from nurse training to the Queensland Eye Hospital and credits their comprehensive new graduate programme with inspiring him to stay in ophthalmology. The theatre-based programme appears comprehensive. Billy was a fine example of the OEH’s goal of “growing their own ophthalmic nurses”. See, it comes back to food again - with the right nutrients, minds will grow.
A less formal, but just as inspirational approach to education needs (feeding minds), was discussed by Cheryl Moore from NSW when she outlined their education via teleconference session, Embracing Distance Learning, TeleC. These one-hour sessions are perfect to link into, no matter how remote or rural one’s location. They’ve been going since 2015 and have covered a wide range of subjects. Us Kiwis in the audience are keen to see how we can start such sessions over here.
Ways to increase interest in ophthalmology were raised during Tongan Mele Vuki‘s discussion on the International Agency for the Prevention of Blindness (IAPB) global ophthalmic nurse-initiated projects. Mele invited Heather Machin, Lynne Hadley, Lo Vola from Fiji and Kiwi Sue Raynel to discuss Where to for ophthalmic nursing? The answers can be summed up as: get involved, get together and make your voice heard. Employers’ encouragement helps too of course. Those of us from Auckland District Health Board appreciate all the support we get from our charge nurses, nurse educators and colleagues. Talking to other nurses from elsewhere, they often do not have the same support.
AONAVIC’s many talks all offered up food for thought. Examples include, Victorian nurse Mitchell Wilson’s WAEH Enucleation Education Project presentation advocating for more holistic and comprehensive support for patients undergoing enucleation. Titch Chan reviewed Rotorua Eye Clinic’s study, underaken using an app, on the cost of care in a cataract theatre and intravitreal injection lists in her presentation Greener Cataracts – values-based medicine app. This is a carbon footprint monitoring app that I believe we should all be using to review efficiency and waste. Check it out Eyefficiency for cataract and intravitreal in the Apple app store.
Thank you to Heather and the rest of the organising team, especially Colleen Flanders who was perfect on the tech side. In summary: great conference!
Don’t forget the next one, the NSW AIONA conference on 9 November in Sydney, linked with the RANZCO meeting.
Olga Brochner is a clinical nurse specialist (CNS) in ophthalmology with the Auckland District Health Board based at the Greenlane Eye Clinic.