PRP and DR and anti-VEGF injections, DMO and agitation research review
Effect of panretinal photocoagulation on corneal sensation and tear function in patients with DR
H Jamali et al
Retina 2021;41:338-344
Review: This study evaluated the effects of panretinal photocoagulation (PRP) on corneal sensation and dry eye signs in patients with diabetic retinopathy (DR). Fifty patients with type 2 diabetes who required PRP were evaluated. Corneal esthesiometry, tear film breakup time, Schirmer’s test and corneal staining pattern were evaluated at baseline and two months after the last PRP session.
Eighty-eight eyes of 50 patients were analysed. The mean tear breakup time decreased from 9.51 seconds at baseline to 7.66 seconds after PRP (p<0.001). Post-PRP eyes also showed more advanced grades of corneal staining and the average value of their Schirmer’s test was 14.39 versus 12.29mm without anaesthesia and 8.18 versus 7.15mm with anaesthesia (p<0.001 for both), for baseline versus post-PRP measurements respectively. Corneal sensation was also reduced after PRP treatment.
Comment: Poor diabetes control contributes to DR, which is the leading cause of blindness in the adult working age. Additionally, diabetic microvasculopathy can lead to diffuse neuropathy, with resultant decrease in corneal sensation and secondary dry eye symptoms. Despite being effective in controlling proliferative DR, PRP can augment corneal neuropathy through thermal damage of the suprachoroidal nerves that are responsible for corneal sensation. Although the suprachoroidal nerves’ larger trunks at three and nine o’clock could be avoided during PRP treatment, partial treatment of smaller nerves is inevitable.
This study suggests that dry eye symptoms can be caused or worsened by PRP treatment and should be discussed with patients before treatment. Artificial tears should also be considered after PRP treatment, particularly for patients with pre-existing ocular surface problems.
Visual acuity outcomes and anti-VEGF therapy intensity in DMO: a real-world analysis
TA Ciulla, JS Pollack, DF Williams
Br J Ophthalmol 2021;105:216-221
Review: This retrospective analysis looked at the relationship between visual acuity outcomes and anti-VEGF treatment intensity in patients with diabetic macular oedema (DMO) across 28,658 treatment-naive eyes from 2013 to 2018.
At one year, a mean of 6.4 anti-VEGF injections were given, resulting in a +4.2 letter visual acuity gain. Less than 20% of patients received monthly injections (10-13 injections) and 50% of eyes received six or fewer injections. Mean letters gained at one year generally showed a linear relationship with mean number of anti-VEGF injections, suggesting that patients who had more frequent treatment see better. Avastin (bevacizumab) was used in about half of all intravitreal injections.
Eyes with good baseline vision (6/12 or better) were at more risk of visual acuity loss at one year, while those with moderately severe baseline visual impairment (6/21 to 6/60), who received 10 or more injections in a year, improved by a mean of +10.3 letters.
Comment: Compared to the results of clinical trials, where anti-VEGF treatment is regimented and frequent, the real-world outcomes of patients with diabetic macular oedema is less favourable, due to less stringent anti-VEGF treatment protocols. This study shows that visual outcomes correlate with treatment intensity at one year and the group at greatest risk of vision loss seems to be patients with good baseline vision (6/12 or better) who are under-treated. These results highlight the necessity for adequate patient counselling about treatment frequency and the unmet need for longer duration therapies that can address the real-world treatment burden.
Agitation of the syringe and release of silicone oil
CDS Dias Junior et al
Eye 2020;34:2242-2248
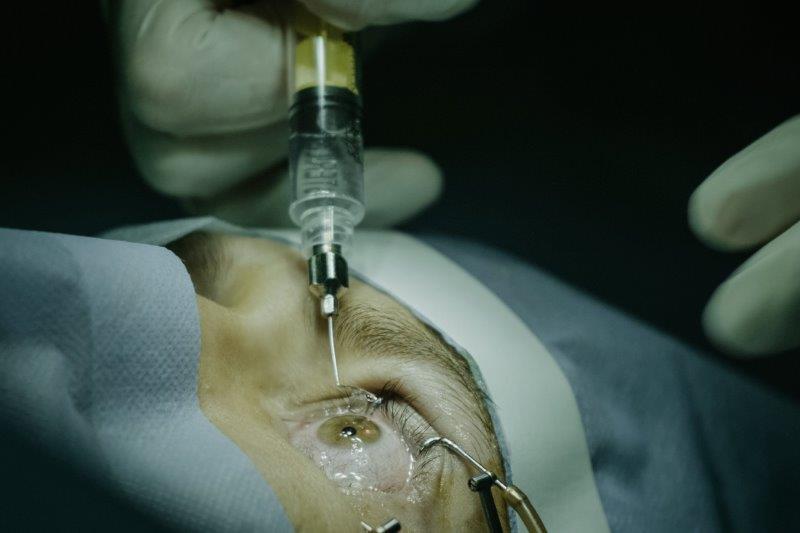
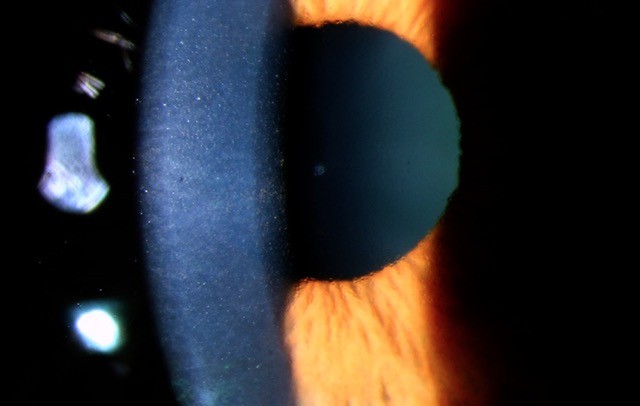
Review: This study sought to investigate whether agitation promotes the release of silicone oil droplets in different syringes used for intravitreal injections. The number of intravitreal injections has increased significantly and virtually all brands of syringes use silicone oil on their inner walls to, among other purposes, facilitate plunger gliding during injection. This silicone oil can be released into the vitreous as droplets during intravitreal injections and it is not uncommon to see this in clinical practice, particularly among patients who have had numerous intravitreal injections.
Two hundred and forty syringes (eight different models) were analysed regarding their release of silicone oil, with or without agitation. Fourier-transform infrared spectroscopy (FTIR) was performed to identify the molecular compounds inside the syringes. Agitation by flicking had a 265 times greater risk of creating oil droplets, when compared with syringes without agitation. Analysis of the tip of the rubber plunger by FTIR indicated the presence of silicone oil in all syringe models.
Comment: With the increasing number of intravitreal injections being performed, individuals with visually significant and symptomatic silicone oil droplets in their vitreous cavity will be more commonly encountered. These droplets could also form complexes with various proteins that could potentially invoke an immune and inflammatory reaction, with the most severe reaction being non-infectious or sterile endophthalmitis. As all of our current injection syringes contain silicone oil on their inner wall, care to not agitate or flick the injection syringe is a worthwhile endeavour.
Dr Joel Yap is a consultant ophthalmologist specialising in retinal diseases and vitreoretinal surgery, with a particular interest in clinical research and secondary intraocular lens implantation. He’s based at Eye Institute, Eye Doctors, ADHB and Counties Manukau DHB in Auckland.