The epidemiology of dry eye disease
Dry eye disease (DED) as a highly prevalent and often debilitating condition has recognised impacts on ocular comfort, visual function, work productivity, psychological well-being and quality of life¹-³. The 2017 TFOS DEWS II Epidemiology report highlighted the paucity of studies in the literature investigating the risk factors and natural history of DED.
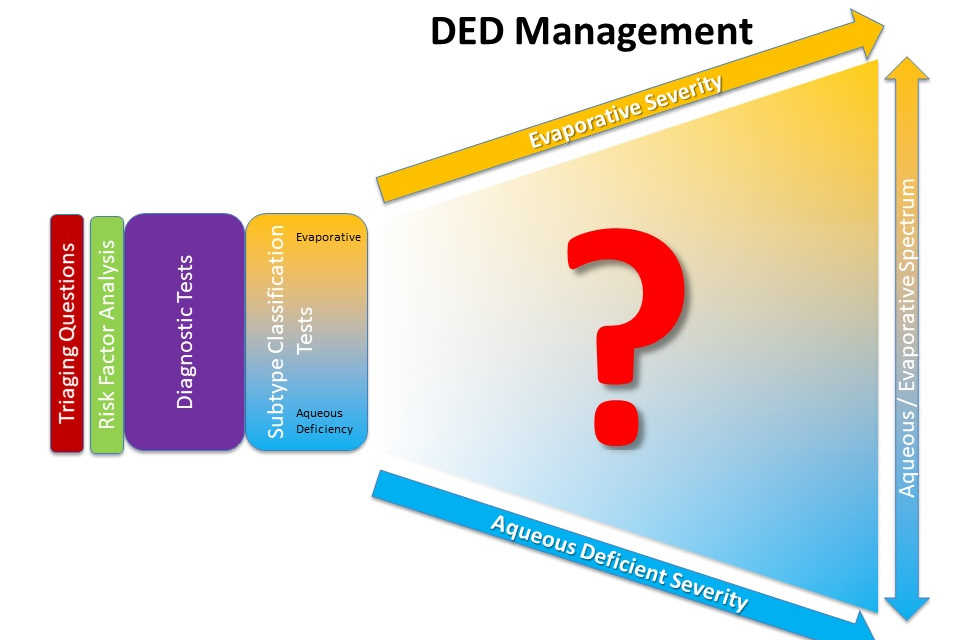
As part of my PhD studies within the Ocular Surface Laboratory (OSL), we assessed the systemic risk factors of DED subtypes in a cohort of 372 community residents, using the global consensus TFOS DEWS II diagnostic criteria⁴. Multivariate regression analysis showed that systemic rheumatological disease and antidepressant medication use were associated with increased odds of aqueous tear deficiency. Independent risk factors for meibomian gland dysfunction (MGD), the primary cause of evaporative dry eye disease, included advancing age, East Asian ethnicity, migraine headaches, thyroid disease and use of oral contraceptive therapy. These results highlight the importance of eye care practitioners routinely enquiring about systemic health when evaluating patients with DED. Opportunistic screening and timely inter-disciplinary referral, arising as a result of such inquiry, would then enable optimisation of modifiable systemic risk factors, including disease activity and medication use, wherever necessary.
Our associated, second study evaluated the impacts of ageing on the natural history of DED in a cohort of 1331 community residents⁵. In agreement with the trends reported in previous studies, the results demonstrated positive associations between ageing and clinical markers of DED, aqueous tear deficiency and MGD. On average, each decade of life was associated with 25% increased odds of developing dry eye disease. Of note, clinical signs of MGD emerged earlier in the natural history of DED progression, with the optimal prognostic cut-off ages for meibomian gland dropout, reduced meibum expressibility and diminished tear film lipid layer thickness occurring in the third decade of life, between the ages of 24 to 29 years. Interestingly, a transient delay was detected between the appearance of clinical signs of MGD and other markers of DED, including tear film instability, hyperosmolarity, lid wiper epitheliopathy and dry eye symptoms, which predominantly emerged during the fourth decade of life, between the ages of 33 and 38 years. This brief delay potentially represents a degree of functional reserve in the ocular surface, as well as a potential window of opportunity for preventative intervention in the younger adult group to attempt to halt the progression of DED. Finally, and of importance to clinicians relying on ocular surface staining in dry eye diagnosis, corneal and conjunctival staining were among the last clinical signs of DED to emerge in the natural history of progression. Such signs of ocular surface damage typically arose between the ages of 46 and 52 years and were more likely to represent moderate-to-severe dry eye disease.
References
- Stapleton F, Alves M, Bunya VY, et al. TFOS DEWS II Epidemiology Report. Ocul Surf. 2017;15(3):334-365.
- Uchino M, Schaumberg DA. Dry Eye Disease: Impact on Quality of Life and Vision. Curr Ophthalmol Rep. 2013;1(2):51-57.
- Belmonte C, Nichols JJ, Cox SM, et al. TFOS DEWS II Pain and Sensation Report. Ocul Surf. 2017;15(3):404-437.
- Wang MTM, Vidal-Rohr M, Muntz A, Diprose WK, Ormonde SE, Wolffsohn JS, Craig JP. Systemic risk factors of dry eye disease subtypes: a New Zealand cross-sectional study. Ocul Surf. 2020;18(3):374-380.
- Wang MTM, Muntz A, Lim J, Kim JS, Lacerda L, Arora A, Craig JP. Ageing and the natural history of dry eye disease: a prospective registry-based cross-sectional study. Ocul Surf. 2020 Aug 3; doi: 10.1016/j.jtos.2020.07.003. Online ahead of print.
Dr Michael Wang is a neuro-ophthalmology clinical research fellow and a PhD student in the Department of Ophthalmology at the University of Auckland.